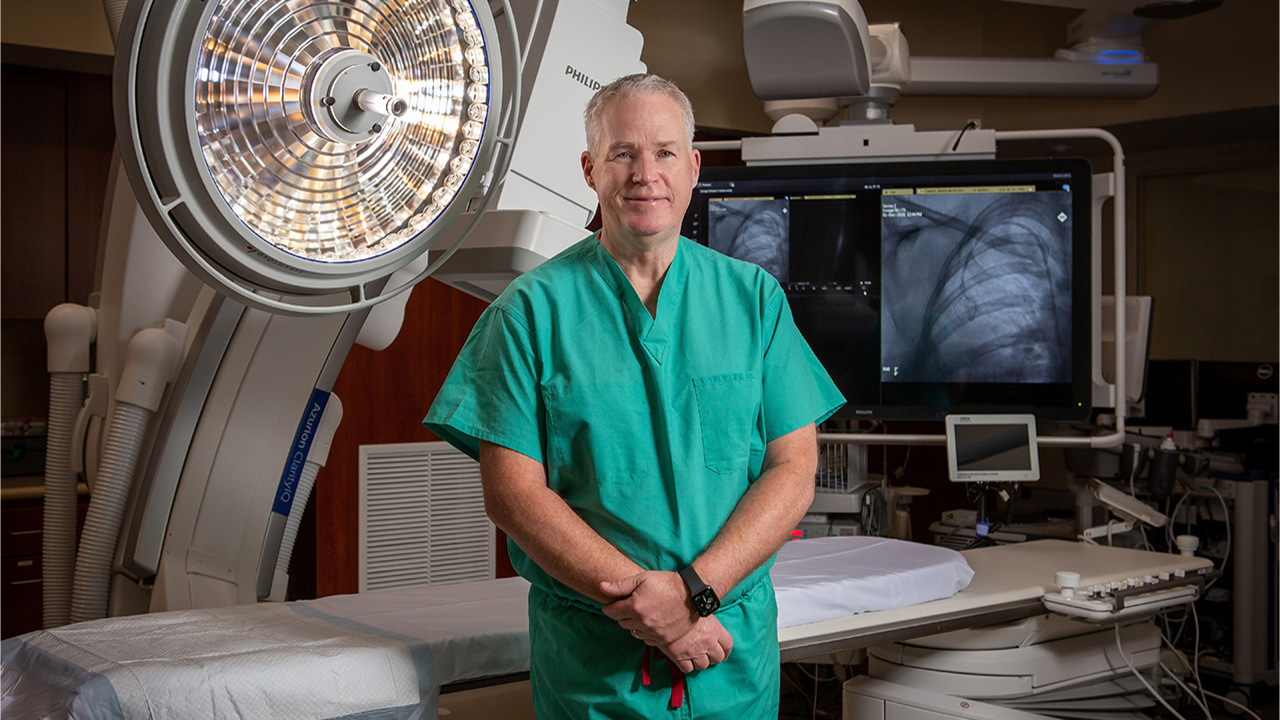
Everything about Joseph McGinn’s first cardiac surgery as a resident at Long Island Jewish Medical Center stays with him. He recalls the heart being packed with ice and stopped, the sound of the heart-lung machine that sustained the patient’s life—and the steady, measured pace about which the head surgeon calmly did his job.
“At the end of the surgery, the patient’s heart popped back into action,” McGinn remembers. “Four days later, the patient was discharged. It was such a dramatic experience for me.
“To this day, I still can’t believe what I do for a living. I can’t believe that I operate on people’s hearts.”
But it’s not just what he does, it’s how he does it that continues to distinguish the chief of cardiac surgery at Miami Cardiac & Vascular Institute, part of Baptist Health South Florida.
The son of a “mad scientist,” a nephrologist (specializing in kidney conditions) who practiced mostly in Staten Island and became a pioneer in renal dialysis, McGinn has followed in his father’s innovative footsteps. In 2005, he debuted a minimally invasive coronary artery bypass grafting procedure (CABG) after which he’s now named. Over the past 18 years, he’s performed more than 7,000 operations using the McGinn Technique.
Among the benefits of minimally invasive bypass surgery compared to traditional sternotomy procedures—in which the breastbone is sawed in half to access the arteries? Patients are back to normal a little more than a week after the operation. Sternotomy patients face months of painful recovery.
And yet, McGinn remains one of few physicians in the United States who sees minimally invasive surgery as a first bypass option. He shares the technique’s origin story—and explains why more surgeons aren’t following in his footsteps—in this interview with Lifestyle.
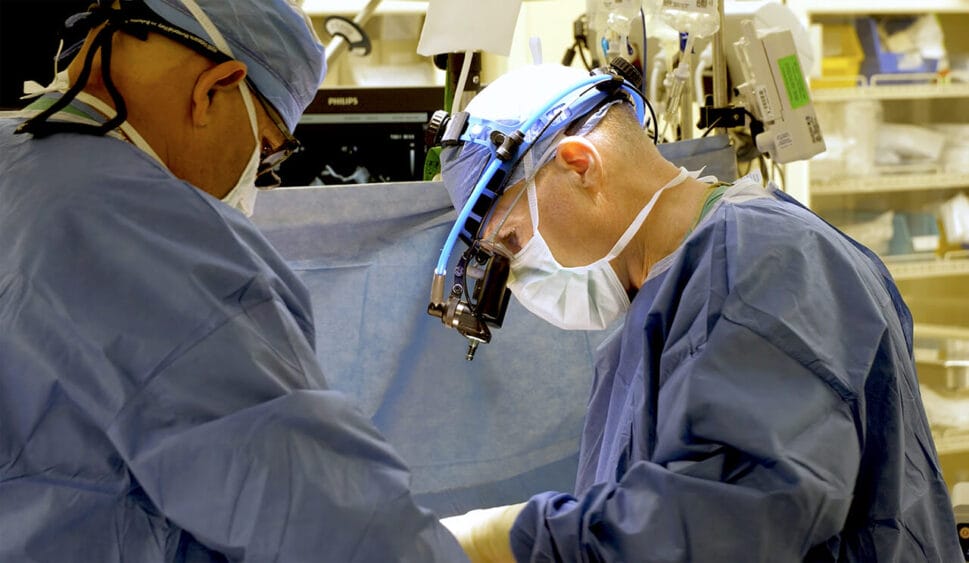
As you were charting your medical course, what drew you to the heart as a specialty?
I looked at the heart initially as a field that was too challenging. No way I could do that. My original calling was to become a renal transplant surgeon [kidney replacement, following somewhat in his father’s discipline].
But then, as part of my training to become a transplant surgeon, I did a rotation in cardiothoracic surgery and I thought, “I can definitely do this.” [Note: McGinn earned his medical degree at State University of New York Downstate Medical Center College of Medicine.]
I loved the idea that I could help a frightened, vulnerable person—and after I’ve performed heart surgery on them and they recover, they’re back home and feeling normal. It’s one of the most rewarding things you can do in medicine.
The heart is literally the organ that gives us life. Do you feel that responsibility, that gravity, before each heart surgery?
Absolutely. I take my job very personally. Maybe to a fault. Because when my patients do well, I’m so excited. And when they don’t do well, it’s the opposite. But it’s also the reason that I went into this field. I wanted to make a difference. It’s a risky surgery. There are high stakes. But the gains are equally as high.
How does someone know that they have the aptitude to perform complex heart surgery at the highest level?
It’s a good question. The successful cardiac surgeons around the world have the ability to look objectively and critically at their outcomes. If you can’t do that, you’ll never succeed. You have to be able to look at your own abilities—and criticize them. That’s only way you get better. At least that was the key ingredient for me.
I consider anyone in this field a constant work of art that’s always being improved. After every case, I’ll look at it and think, OK, maybe I can try this next time. I think that’s part of my innovation side. I want to find a better way of doing something.
And there’s always a better way.
In traditional cardiac bypass surgery, the breastbone is broken to access the heart, and patients have that long incision scar on the chest. What was troubling to you about the procedure?
I watched all the specialties around me evolve. I’m talking about orthopedic surgery, gynecology surgery, general surgery. They all evolved from doing open surgery to laparoscopic procedures or arthroscopic surgery for knees, and so on. All of these fields were changing from big, open incisions to something smaller.
But cardiac surgery never made that move for whatever reason. It intrigued me to figure out why it never happened—and what I could do about it.
I also thought that there was a certain group of patients who were not [being treated with] heart surgery because it was too invasive—they were too old or they had other medical problems, and it would be too much for them to go through another big surgery. As part of the medical community, I felt compelled to figure out a less-invasive approach for that group of patients—because otherwise, they would have been left out.
What are the issues with traditional bypass surgery that patients may experience?
The big issue is pain [during the recovery], but it’s more than that. The problem also is that when you cut a large bone like the breastbone—one of the biggest in the body and a source of a lot of bone marrow—it can take two or three months for that bone to heal solidly. All the energy that’s devoted to the healing of the bone is taken away from somewhere else. That has a huge impact on the body’s functioning.
If you take someone who has an ongoing chronic illness—let’s say, diabetes that’s out of control, or chronic bronchitis from smoking—those patients already are disabled and having problems. When you add a big incision from heart surgery, you’re compounding the issue. It’s a big deal for them to heal, and the pain from the incision causes disability. It forces them to be more sedate and not walk around, and that has its own physiological impact.
My goal was to figure out how to deliver the same long-lasting result but do it in a way that doesn’t have such a negative impact on the patients.
How did you arrive at the procedure that now bears your name?
I have a close friend who works at a company that was dabbling with a gizmo called a heart positioner. The heart is tethered by all the vessels on the right side, so you can move the left side around pretty well—and this positioner did that. Wouldn’t it be great, he said, if we could figure out a way of doing minimally invasive heart surgery with the help this positioning device?
He called me out to Minnesota. We had some cadavers, we had some pigs, and we started working on it. We were trying different incisions, different approaches. And we clicked on the approach that we use today. This was 18 years ago. [After going through FDA and approval processes], we did three or four live cases toward the end of 2005.
As the engineering has improved and the equipment has been adapted to the application, I’m now basically doing every case this way. I do maybe two or three surgeries a year where [he’s going through the sternum].
Could you give us a layman’s version of what the procedure actually entails?
We usually make about a 2.5-inch incision on the left side [the window incision], just below the nipple of the breast, and we go in between the ribs. [Note: Two other tiny incisions serve as access ports.] We deflate the left lung, so it’s out of the way, and that gives us access to the heart.
As I mentioned before, the heart is connected mostly on the right side. The left side is free to move around. Using a device with a suction cup at the end of it, I can l rotate the heart so that the artery I need to bypass comes right into the window incision, and then I create the bypass the way I would do it through a sternotomy.
The left-side incision angle is beneficial because most of the arteries are on the left side; it’s where all the main action is. So, we only have to rotate the heart a little bit to get to the arteries in the back or front of the heart.
The big difference is that in a sternotomy you make a huge incision—and you rotate the heart a ton—to get directly to the arteries in the back of the heart. In this minimally invasive procedure, we bring the artery to the incision.
Were there challenges that you had to solve along the way?
There’s no progress made without significant challenges. If there were no challenges, it would’ve been done long before. So, yes, there were engineering issues, technical issues, procedural issues that we had to work out.
When I got to Baptist three years ago, in working with some of the teammates, we found that there was a better way of doing it. So, we slightly changed the procedure, allowing us to complete the surgery in even less time. That limits the amount of anesthesia and makes for a more efficient procedure.
But the basic technique has been much the same for the past 10 years, with little tweaks here and there.
Beyond the diminished pain during recovery, what are the benefits for patients?
All of my patients stay in the hospital about three or four days. Then they have three or four days of convalescing at home. And then they go back to full daily activities—that means driving, golfing, swimming.
With traditional bypass surgery, you’re looking at a minimum of two months for recovery.
I’m asking patients to lay low for eight days.

Why is the surgery only performed in a handful of hospitals in the U.S.?
I do most of the teaching for it, so I have surgeons visit me to try and learn how to do the procedure. Maybe 1 out of 20 actually decide to use it. There’s a very long learning curve. The initial surgeries, when I first started doing them, would take me six hours, maybe seven, for a double bypass. Now, it takes me three hours for a double bypass. But it took [years] to get through that learning curve, and a lot of surgeons don’t have the patience for that.
Is that disappointing to you given all the benefits for the patient?
I am disappointed. I’m working to see if we can’t figure out a better strategy for educating other surgeons in the U.S. on how to do the procedure. The interesting thing is that in Asia—India, Japan, China, Singapore, Malaysia—they’re all doing this procedure pretty regularly. It may be financially driven [in those countries] since patients get home and back to work sooner.
But I do wish it was adopted more in the United States.
Do you have patients who, through their own research, seek you out?
About 60 to 70 percent of my schedule involves patients from outside of South Florida.
One of my first patients came from Texas. He owned a plumbing company and had one apprentice working with him. He had two college tuitions and a mortgage to pay. If he didn’t work, he wasn’t going to make those obligations. So, he sought an alternative to the traditional sternotomy. We did a triple mixed [coronary artery bypass grafting] on him, and he was back to work seven days after getting out of the operating room.
I always say that we’re so grateful to help patients live a better life, because that’s our goal. But we never think of the financial side. That was a chance for me to save someone’s financial life, which was something I’d never thought much about.
As I’m doing this more and more, I see how many patients live paycheck to paycheck. We’re not getting billionaires coming in every day. These patients can’t afford to be out of work for three months. So, for us to provide an alternative, it’s very meaningful for most patients.
Are there additional innovations that you’re exploring?
We’re putting together a combination of two innovations—trans-catheter aortic valve replacement [TAVR] and coronary artery bypass grafting. Right now, if a patient with blocked arteries and an aortic valve problem comes to any hospital in the U.S., they’re going to get an open-end operation, coronary bypass and a surgical valve replacement. They’re going to be laid up for three months. And it’s one of the highest risk operations we do as heart surgeons.
We’re trying to combine a minimally invasive coronary bypass with a TAVR and accomplish the same end point—fix the valve and bypass the arteries. Yet the hospitalization will be about three or four days, and the overall recovery seven or eight days.
One of the early patients we did was a young lady with breast cancer who was going through chemotherapy. During treatment, doctors found she had aortic stenosis and coronary artery disease. Under normal circumstances, given the debilitating effects of the chemo, she couldn’t tolerate those surgeries. But she could tolerate a TAVR, which we did. Two days later, we did a minimally invasive bypass. Three days later, she went home. A week after that, she started back on her chemotherapy.
That treatment could not happen in any other hospital in the United States. Or any other country for that matter. We’ve done five more cases since.
Photos courtesy of Baptist Health South Florida